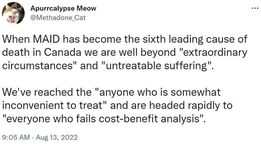
I ASKED “GROK” IF THIS STATEMENT WAS TRUE AND RECEIVED THIS RESPONSE…
Yes, the claim is largely true, based on a new Medicare pilot program launching January 1, 2026, in six states (Arizona, New Jersey, Ohio, Oklahoma, Texas, and Washington). This program introduces AI-assisted prior authorization for certain treatments in traditional Medicare (Parts A and 😎, with private contractors incentivized financially for denying or reducing “wasteful” care. While the final denial decision requires human clinician review and there’s an appeals process, critics—including doctors, lawmakers from both parties, and patient advocates—argue the structure heavily favors denials, potentially delaying or blocking essential care for seniors. Below, I’ll break it down with key details.
The Program: WISeR Model
• What it is: The Centers for Medicare & Medicaid Services (CMS) is rolling out the Wasteful and Inappropriate Service Reduction (WISeR) Model, a six-year pilot aimed at curbing fraud, waste, and abuse by requiring prior authorization for high-cost, low-value procedures (e.g., knee surgeries, nerve stimulation for pain, or incontinence treatments). Private companies will use AI algorithms to review requests and flag potential denials.
• Private firms’ role: CMS contracts with for-profit vendors like Humata Health (backed by Blue Cross Blue Shield and UnitedHealth investors), Innovaccer (linked to Kaiser Permanente), and Virtix Health. These firms analyze patient data via AI to assess “medical necessity” against Medicare guidelines.
• Payment incentives: Contractors earn a share of “averted expenditures”—savings from denied or shortened care—creating a direct financial reward for rejections. CMS claims safeguards like penalties for wrongful denials and human oversight, but experts call this a “bounty hunter” setup that biases toward cost-cutting.
• Scope: It affects millions of traditional Medicare beneficiaries (not just Medicare Advantage plans) in the pilot states, with automatic enrollment for Parts A/B users. No opt-out option exists, though appeals are available (success rate ~82% in similar systems, but often delayed).
Evidence of AI-Driven Denials
• Existing issues in Medicare Advantage: Private insurers (e.g., UnitedHealth, Humana) already use AI tools like NaviHealth’s nH Predict algorithm to deny post-acute care (e.g., nursing home stays). A 2023 STAT investigation found these tools predict “length of stay” and cut coverage prematurely, even for patients with cancer or amputations—leading to lawsuits and a 2024 Senate report showing denial rates 16x higher with AI. In one case, a 74-year-old woman was discharged after 17 days (per AI prediction) despite needing more rehab, forcing her to drain savings.
• Pilot risks: Doctors report 93% of prior authorizations already delay care; AI could worsen this, with 82% leading to treatment abandonment. A 2022 HHS probe found 13% of Medicare Advantage denials were improper. Critics fear the pilot will expand this to traditional Medicare, overriding doctors for profit—echoing “death panels” fears.
Reactions and Pushback
• Bipartisan opposition: Over 30 House Democrats introduced the Seniors Deserve SMARTER Care Act in November 2025 to block it, citing profit-driven barriers. Sen. Patty Murray (D-WA) called it a “backdoor move to privatize Medicare.” Even some Republicans and groups like the American Medical Association warn of harm.
• CMS defense: Officials say AI speeds approvals (target: 72 hours) and ensures “appropriate” care, with no direct tie to denial volume. But transparency is low—algorithms are proprietary, and vendors have insurer ties.
• Broader context: This builds on Medicare Advantage trends, where private plans (54% of seniors) deny 6-25% of requests, often via AI, while overbilling CMS $84 billion in 2025 (per MedPAC). Appeals succeed but can take months, outlasting patients.
Is It Overstated?
The claim’s phrasing is alarmist (“AI decides who gets treated”), but not baseless—AI heavily influences decisions, and incentives prioritize denials. Traditional Medicare has avoided prior auth for 60 years to prevent exactly this; the pilot tests privatization risks. If you’re in a pilot state, consult your doctor early for appeals prep, and contact reps to support blocking legislation.
For more: Check CMS’s WISeR fact sheet or the STAT series on AI denials. This isn’t hypothetical—it’s set to start in three weeks.
In Album: AmericanPride's Timeline Photos
Dimension:
1080 x 1350
File Size:
186.17 Kb
4 people like this.

tambourinegirl, Den, MAFury, TexasJerryLee reacted this

TexasJerryLee
Gut the federal government. Seems to be the only way to save the Republic!


JimJimmyJames
This meme is a bit dated. MAID has become the 4th leading cause of death in Canada.